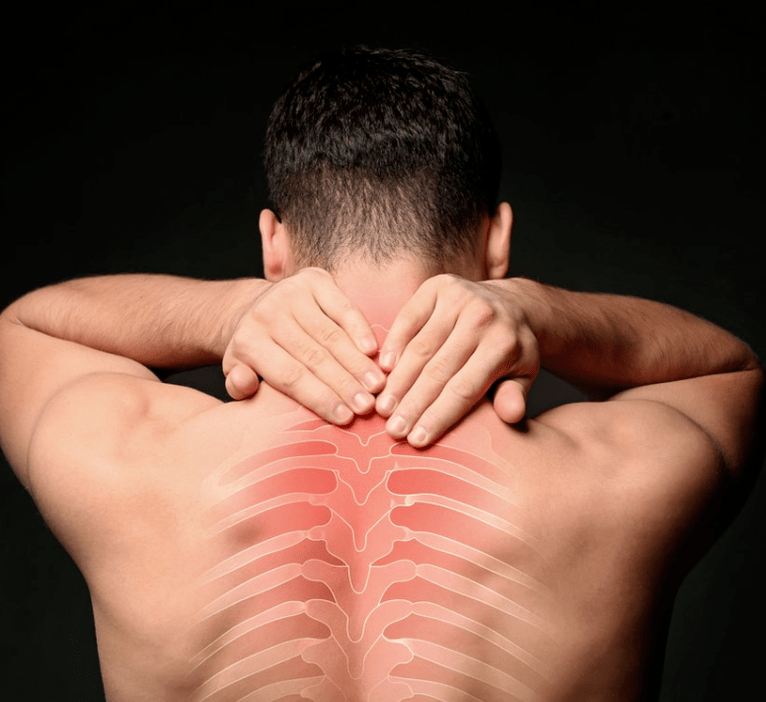
Osteochondrosis is the most common disease of all spinal diseases. Since osteochondrosis is directly a dystrophic-degenerative lesion of the discs located between the vertebrae, then, as a result, this leads to an irreversible change in their structure, as well as in the shape of the discs themselves, which make up the thoracic spine.
With an increase in a person's age, these changes in his spine develop more and more, and by the age of about 40-45 years, almost everyone suffers from osteochondrosis of the spine. By itself, osteochondrosis of the thoracic spine develops much less often than, for example, the lumbar or cervical spine, since the vertebrae in it are much less mobile than in other vertebral zones. In addition, the back area in the chest area has a more developed corset of muscles, which supports the spine in the thoracic region much better than in others.
What is this thoracic osteochondrosis?
Chest osteochondrosisdirectly represents a stratification of discs between the vertebrae with a simultaneous decrease in their thickness and, as a result, the subsequent pinching of the nerve endings located in the intercostal zone of the human chest.
However, we note once again that in view of the fact that physiological fixation by the ribs in humans is rather rigid, the spine in the chest area is least susceptible to osteochondrosis. It is thoracic osteochondrosis that is a rare phenomenon in relation to, for example, osteochondrosis of the cervical or lumbar.
Usually, with osteochondrosis of the thoracic spine, the discs between the vertebrae of the thoracic spine, which includes twelve thoracic vertebrae, are involved in the pathology process. But most often with osteochondrosis of the thoracic region, pathological changes occur with the upper thoracic vertebrae. There are several degrees of lesion with thoracic osteochondrosis, and further we will consider them in more detail.
Predisposing factors for the development of thoracic osteochondrosis
The exact causes of the occurrence of osteochondrosis of the thoracic region have not yet been fully established by modern science. At the moment, it is customary to distinguish in medicine the following predisposing factors, or the so-called risk factors, due to which osteochondrosis of the thoracic region occurs in the spine:
- hereditary predisposition;
- excessive physical activity in this part of the spine;
- spinal injury, such as falls or bruises in the thoracic region;
- changes that occur with age in the intervertebral discs, and lead to a decrease in hydration in the tissues of the discs;
- violations of blood supply in the chest area.
Causes contributing to the disease of thoracic osteochondrosis
In the main, the development of the disease with osteochondrosis is generally promoted by hypodynamia, that is, a lack of muscle loads, leading to a weakening of the functions of the muscular corset and, as a result, to an increase in loads on the intervertebral discs and ligaments.
Additional reasons for the development of thoracic osteochondrosis are:
- hypothermia of the body;
- the presence of chronic stressful situations;
- transferred infections;
- difficult conditions of physical labor;
- arisen hormonal disorders in the body;
- violation of the metabolic process in the body;
- the presence of congenital defects of the spine, namely its thoracic region.
In the course of exposure to a combination of these factors, or sometimes even one, dystrophic-degenerative irreversible processes develop in the discs between the vertebrae over time:
- the nucleus pulposus of the intervertebral disc gradually begins to lose fluid, which was secreted by them to provide a lubricating function, which ultimately significantly reduces the damping function of this disc;
- the fibrous ring of the vertebrae themselves, due to the increased load on it, becomes more vulnerable, which in turn leads to its gradual destruction.
Symptoms and signs of thoracic osteochondrosis of the spine
The clinical symptoms of thoracic osteochondrosis depend entirely on the following factors:
- the patient's age;
- the degree of disease affection;
- stages of osteochondrosis of the thoracic spine: remission or exacerbation.
The main signs of thoracic osteochondrosis are:
- pain in the chest in the spine, the so-called dorsago;
- painful damage to the nerve endings of the spinal cord - radiculopathy;
- abdominal syndrome;
- cardiac syndrome or changes in the heart muscle, with characteristic pains that persist even under the influence of trinitroglycerin;
- pulmonary syndrome, in the form of stagnation in the lungs with signs of hypoxia, that is, suffocation.
An increase in body temperature in a patient with thoracic osteochondrosis is not observed, which is also a direct differential diagnostic sign. Dorsalgia in the chest area as one of the main symptoms of osteochondrosis indicates the occurrence of cracks in the annulus fibrosus and deformation of the nucleus pulposus. When palpating, the pain in this area of the chest only intensifies, the symptoms increase.
In addition, the characteristic symptoms of thoracic osteochondrosis with compression myelopathy, that is, deformation of the nerve endings, are:
- feeling of "goose bumps" - paresthesia;
- pain along the compressed nerve - are common symptoms;
- decrease in sensitivity to temperature and from touch;
- disorders of the motor function of the spine are also one of the characteristic symptoms.
Having found such symptoms, you need to see a specialist. The appearance of symptoms in the complex and their intensity are especially dangerous. At the same time, it is inappropriate to treat the symptoms without eradicating the causes and factors of the disease.
Degrees of the disease with thoracic osteochondrosis
Each degree of the disease with thoracic osteochondrosis is characterized by its own pathology, which has only its own clinical signs. Modern medicine distinguishes four degrees of degenerative disc disease of the thoracic region (similarly - lumbar and cervical degenerative disc disease) and, accordingly, four periods of its development. Let's consider them in more detail.
First degree,for which it is characteristic that cracks appear inside the fibrous ring, into which the nucleus pulposus subsequently penetrates. This period of development of the disease with thoracic osteochondrosis is characterized by the following symptoms:
- the appearance of pain in the spine that does not go beyond the localization of the lesion;
- these pains can be either permanent or be expressed by lumbago;
- there may be a convulsive contraction of the muscles in the thoracic region, accompanied by pain in the heart region.
Second degreethe development of thoracic osteochondrosis is characterized by the pathological occurrence of increased intervertebral mobility with the following clinical manifestations:
- subluxations appear in the thoracic spine;
- pain increases during movement;
- discomfort appears with prolonged posture.
Third degreecharacterized by rupture of the annulus fibrosus and the exit of the nucleus pulposus beyond its limits. In this period of the disease with osteochondrosis of the thoracic spine, intervertebral hernias begin to appear, the clinical signs of which are rather severe. Namely - neurovascular, muscle-tonic and reflex-dystrophic.
In addition to the above, for the third degree of osteochondrosis of the thoracic region, a change in the following conditions of the spine is characteristic:
- weak fixation of the position of the spine;
- limitation of mobility of the spinal region, manifested in the form of kyphosis or scoliosis.
Fourth degree- the dystrophic-degenerative process already affects all structures that are surrounded by the spine. This pathological process involves the yellow, interspinous and other ligaments, and fibrosis occurs in the structures surrounding the spinal column. In this period of the disease with thoracic osteochondrosis, the so-called state of remission is clinically observed.
Complications
With further progression of the disease with thoracic osteochondrosis, the development of concomitant complications is possible:
- inflammation of the nerve endings of the spinal cord;
- the occurrence of intervertebral hernias;
- development of vascular dystonia;
- the development of Schmorl's hernia;
- spondyloarthrosis disease;
- pathological growth of bone growths - osteophytes;
- a significant decrease in the spinal canal.
It should be noted that the severity of complications arising in thoracic osteochondrosis depends entirely on the rate of progress of the process of the disease that has arisen and, of course, on the effectiveness of methods for treating osteochondrosis of the thoracic spine.
Diagnostics and its methods
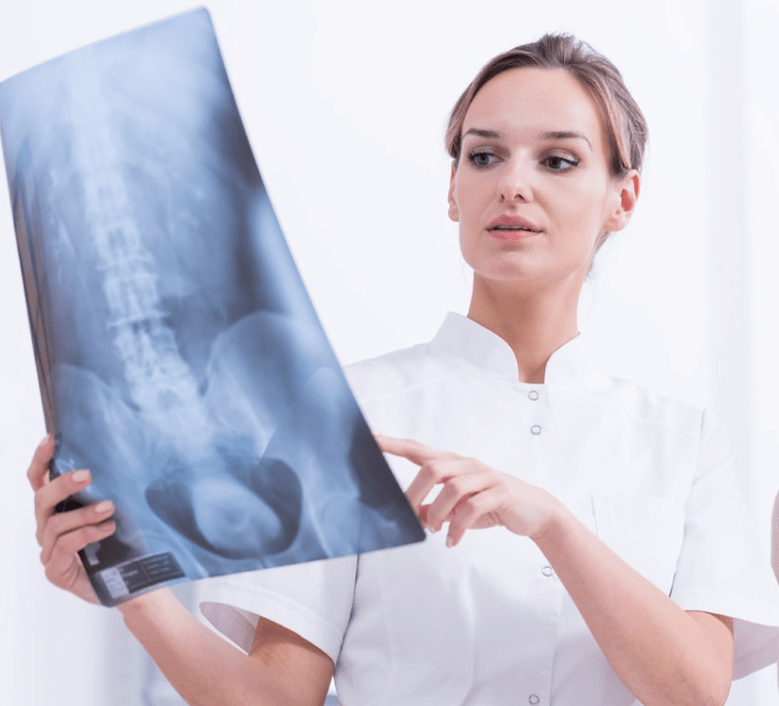
In practice, several methods are used to diagnose thoracic osteochondrosis. Of these, the most common is X-ray examination, the results of which are quite informative. Signs of thoracic osteochondrosis detected in this study are the following:
- the contours of the discs between the vertebrae are broken;
- the edges of the integumentary plates acquired a wavy character;
- the intervertebral discs have changed their shape;
- osteophytes appeared - bony pathological growths in the spine;
- the hook-shaped processes of the vertebrae have increased and sharpened;
- the bodies of the thoracic vertebrae have changed their normal shape;
- the height of the discs between the vertebrae has significantly decreased;
- herniated discs between the vertebrae formed.
In some cases, the method of diagnosing thoracic osteochondrosis of the spine is practiced by means of an X-ray contrast study, which determines the following signs of this ailment:
- in the case of advanced pathology, the contrast agent fills the disc between the vertebrae completely;
- with the help of a contrast agent, the contours of the nucleus pulposus are visible, which are uneven;
- when the intervertebral disc is destroyed, the contrast agent largely penetrates beyond its limits, up to penetration into the spinal canal.
Only the correct diagnosis can determine the correct treatment.
Treatment of osteochondrosis
Treatment of thoracic osteochondrosis is possible in one of the following ways, used taking into account the results of diagnostics of thoracic osteochondrosis, namely:
- conservative-traditional treatment of the spine;
- treatment of chest osteochondrosis with traction;
- operative surgical intervention.
Treatment of chest osteochondrosis, called conservative, is complex for the treatment of any type of osteochondrosis: medications, physiotherapy, physiotherapy exercises. Non-steroidal anti-inflammatory drugs are aimed at relieving pain in the spine, which is known for thoracic osteochondrosis. It should be noted that these medications very well eliminate inflammatory processes, as well as the resulting swelling, helping to reduce the compression of the nerve roots. In more complex cases of breast osteochondrosis, the attending physician may prescribe a number of additional medications, for example, some potent pain relievers and muscle relaxants that block the appearance of muscle spasms.
When the pain recedes or it was managed to stop, that is, during remission, physiotherapy treatment is prescribed, as well as, in addition, exercise therapy and massage. These are all important components of a comprehensive treatment. One of the main physiotherapeutic tools for the treatment and prevention of the disease is pulsed magnetic therapy using special medical devices for clinical and home use.
Only magnetotherapy of special parameters is allowed for use during exacerbations; there are medical devices for dealing with both acute and chronic pain. This system is also suitable for the treatment of the lumbosacral and cervical spine.
In addition to the above, traction treatment, that is, the treatment of chest osteochondrosis by means of special traction, can be successfully used to treat thoracic osteochondrosis. With this method, the paravertebral muscles, tissues and ligaments are stretched, which leads to an increase in the intervertebral distance. Even one and a half millimeters will already be enough to reduce swelling, eliminate compression, as well as relieve tension in the muscles adjacent to the spine. In any case, the main principle of conservative treatment is its complexity. The treatment will have to be done for a long time and regularly, this is the only way to hope for results.
But surgical intervention as a type of treatment for osteochondrosis is advisable only when the above methods of treating chest osteochondrosis do not give the desired result.




































